Our team designs and evaluates public health interventions to address the major causes of maternal and newborn morbidity and mortality in low-income countries.
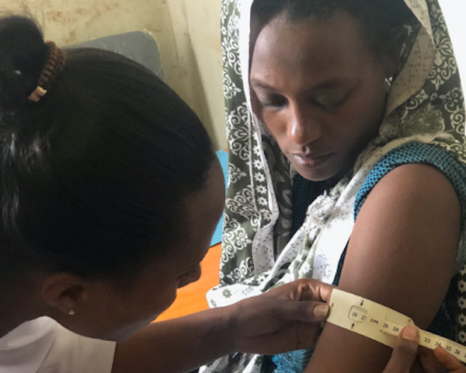
In low- and middle-income countries, infections are common in pregnancy and under-treated due to lack of testing and treatment. Maternal malnutrition is also prevalent in many settings. These factors adversely affect the health of the mother and fetus, and lead to preterm birth and fetal growth restriction. Learn more about our ENAT (“Mother”) Study & child development studies in Ethiopia.
One in five babies do not grow to their optimal potential in the womb and one in eight are born premature. We have been developing methods to improve pregnancy dating, identify vulnerable babies, and testing interventions to prevent preterm birth and fetal growth restriction in low resource settings. Learn more about our studies in Bangladesh and Ethiopia.
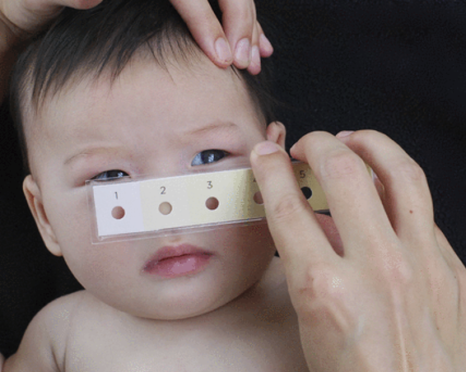
We are designing tools to help frontline health workers manage small and sick babies in low-resource settings. One of our innovations, the Bili-ruler, is a simple, low-cost color matching tool to identify newborn jaundice. We also have developed a mobile phone application for community health workers to assess and manage newborn illness, including prematurity and infections.
We aim to improve evidence of the major causes and outcomes of newborn illness and deaths in low-income settings, where a majority of births and deaths are never recorded. Our epidemiologic research on the global burden of preterm birth, birth asphyxia, newborn infections, and fetal growth restriction has helped influence the Every Newborn Action Plan of the World Health Organization and UNICEF.
We are conducting studies with parents of different racial and ethnic backgrounds to better understand specific barriers and facilitators to breastfeeding. These studies will examine breastfeeding outcomes and lactation support by race/ethnicity at Brigham & Women’s Hospital.
Mama Sana is a culturally appropriate, language-concordant “wrap around” (i.e. providing continuity of pre-and post-natal) care program for Spanish-speaking birthing parents that will deliver nutrition, breastfeeding, exercise, mental health, and infant development education and support.